Laryngopharyngeal Reflux / Gastroesophageal Reflux
Home | Conditions | Laryngopharyngeal Reflux
What is Laryngopharyngeal Reflux (LPR) / Gastroesophageal Reflux (GERD)?
Laryngopharyngeal reflux (LPR) is a condition in which acid that is made in the stomach travels up the esophagus (swallowing tube) and gets to the throat. The terms laryngopharyngeal reflux and gastroesophageal reflux (GERD) are sometimes used interchangeably.
Who Is More Prone To Laryngopharyngeal Reflux?
Anyone can get LPR, but it occurs more often in the older age group. People who are more likely to have LPR include those who have poor dietary habits, consistently wear tight or binding clothing and are overweight or are overstressed.
What Causes Laryngopharyngeal Reflux?
LPR is caused by stomach acid that bubbles up into the throat. When you swallow, food passes down your throat and through your esophagus to your stomach. A muscle called the lower esophageal sphincter controls the opening between the esophagus and the stomach. The muscle remains tightly closed except when you swallow food.
When this muscle fails to close, the acid-containing contents of the stomach can travel back up into the esophagus. This backward movement is called reflux.

What Are Some Symptoms Of Laryngopharyngeal Reflux?
The symptoms of LPR are felt in the throat and include the following:
- Sore throat
- Hoarseness
- Sensation of a lump in the throat
- The constant need to clear the throat
- The sensation of mucus sticking in the throat, and/or post-nasal drip
- Chronic (long-term) cough
- Difficulty swallowing
How is Laryngopharyngeal Reflux Diagnosed?
LPR is usually diagnosed based on the patient’s symptoms of irritation or swelling in the throat and the back of the voice box on flexible nasoendoscopy. However, flexible nasoendoscopy can only visualize up to the area of the vocal cords and its surroundings.
If further testing is needed, there are 3 more commonly used tests
- A swallowing study (Barium Study)
- Oesophago-gastro-duodenoscopy (OGD)
- Esophageal pH manometry
Barium Study
In a swallowing study, the patient swallows a special liquid called barium, which coats the esophagus, stomach and intestine so they are outlined on an X-ray. This allows the doctor to see the movement of food as it passes from the mouth to the esophagus, and if any barium reflux occurs into the esophagus after swallowing.
Oesophago-gastro-duodenoscopy (OGD)
An OGD can also be performed, where the inside of the stomach and esophagus can be visualized with an endoscope. Under sedation, this is passed through the mouth, down the esophagus and into the stomach. Changes in the lining of the esophagus and the stomach can then be visualized, and the diagnosis of reflux made.
Esophageal pH manometry
The final test is the esophageal pH test. It measures and records the pH (level of acid) in the esophagus. A thin, small tube with a device on the tip that senses acid is gently passed through the nose, down the esophagus, and positioned about 2 inches above the lower esophageal sphincter. The tube is fastened to the side of the face with tape. The end of the tube that comes out of the nose is attached to a portable recorder that is worn on the belt or over the shoulder. The recorder has several buttons on it that the patient presses to mark certain events. This is usually left in place for 24 hours. This test is able to detect both acid and alkaline reflux, and is the gold standard in the diagnosis of LPR.
How is Laryngopharyngeal Reflux Treated?
Most cases of LPR do not need medical care and can be managed with lifestyle changes, which include:
- Dietary modifications with food low in acid levels, low in fat and spice.
- Eat frequent, small meals.
- Lose weight.
- Avoid the use of alcohol, tobacco and caffeine.
- Do not eat food less than 3-4 hours before bedtime.
- Raise the head of your bed before sleeping. Place a strong, solid object (like a board) under the top portion of the mattress. This will help prop up your head and the upper portion of your body, which will help keep stomach acid from backing up into your throat. The alternative is to sleep on more than one pillow.
- Avoid clearing your throat unnecessarily.
- Medications to decrease acid reflux may be necessary.
In very severe cases of LPR, surgery may be recommended as treatment.

What Can Happen If Laryngopharyngeal Reflux Is Untreated?
If not treated, LPR can lead to:
- Chronic sore throat
- Chronic cough
- Swelling of the vocal cords
- Ulcers on the vocal cords
- Formation of granulomas (benign masses) in the voice box
- Worsening of asthma, emphysema, and bronchitis
Untreated LPR also may play a role in the development of cancer of the voice box.
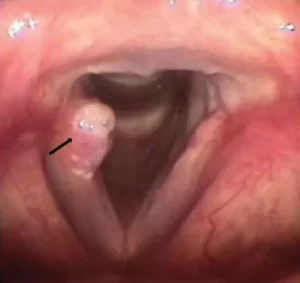
Right granuloma of the vocal cord
Can Laryngopharyngeal Reflux Be Prevented?
To decrease your chance of having LPR, avoid the following:
- Acidic, spicy and fatty foods
- Alcohol
- Tobacco
- Beverages that contain caffeine (tea, coffee, soda, etc.)
- Chocolate
- Mint or mint-flavored foods
Other things you can do to help prevent LPR:
- Do not wear tight or binding clothing.
- Be sure to maintain a healthy weight.
- Avoid eating less than 3-4 hours before bedtime.
- Try to avoid becoming overly stressed. Learn ways to help manage or reduce stress levels.
Voice Conditions
Throat / Swallowing Conditions
Procedures & Treatments
- Tracheostomy
- Microlaryngoscopy with Phonosurgery
- Flexible Nasoendoscopy
- Direct Laryngoscopy
- Removal of ingested foreign body
- Tonsillectomy

